Effect of Diabetes on Oral Health
Diabetes affects your mouth in ways you might not expect. This guide is for people with diabetes, their caregivers, and anyone wanting to understand how blood sugar impacts oral health.
When your blood sugar runs high, your mouth becomes a breeding ground for bacteria and infections. Diabetics face higher risks of gum disease, tooth loss, and slow-healing wounds in their mouth. The connection works both ways—poor oral health can make blood sugar harder to control.
We'll explore the most common oral health problems diabetics face and the warning signs you should never ignore. You'll also learn practical strategies to protect your teeth and gums while keeping your blood sugar in check.



Understanding the Diabetes-Oral Health Connection
How Blood Sugar Levels Directly Impact Your Mouth
Your mouth operates like a delicate ecosystem, and high blood sugar acts like a disruptor that throws everything off balance. When glucose levels spike and remain elevated, your saliva becomes a sugar rich environment that oral bacteria absolutely love. These harmful bacteria feed on the excess glucose, multiplying rapidly and producing acids that attack your teeth and gums.
High blood sugar also reduces saliva production, creating what dentists call "dry mouth." Saliva normally acts as your mouth's natural defense system, washing away food particles and neutralizing acids. Without adequate saliva flow, bacteria build up more easily, plaque hardens faster, and your natural cleaning mechanism fails.
The blood vessels in your gums become another casualty of elevated glucose. Diabetes damages these tiny vessels, reducing blood flow to your gums and other oral tissues. This poor circulation means your mouth receives fewer infection-fighting white blood cells and healing nutrients, making it harder to fight off bacteria and repair damage.
Why Diabetics Face Higher Risks for Oral Complications
Diabetics deal with a perfect storm of factors that increase oral health risks. Your immune system doesn't function at full capacity when blood sugar runs high, making it significantly harder to fight off the bacteria that cause gum disease, tooth decay, and oral infections.
The healing process becomes sluggish too. Minor cuts, scratches, or irritation in your mouth that would normally heal within days can linger for weeks in people with poorly controlled diabetes. This extended healing time gives bacteria more opportunities to establish infections.
Diabetics also experience more severe oral health problems compared to non-diabetics. A simple case of gingivitis can progress to serious periodontitis much faster. Tooth loss rates are higher, and oral infections can become more serious and spread more easily.
Your medication regimen can add another layer of complexity. Some diabetes medications cause dry mouth as a side effect, compounding the saliva reduction that high blood sugar already creates.
The Two-Way Relationship Between Diabetes and Gum Disease
The connection between diabetes and gum disease works both directions, creating a cycle that can spiral out of control if left unchecked. Diabetes makes gum disease worse, but gum disease also makes diabetes harder to control.
When you have active gum disease, your body stays in a constant state of inflammation. This chronic inflammation releases chemicals that interfere with insulin's ability to control blood sugar. Your glucose levels become more unpredictable, and you may need higher doses of medication or insulin to achieve the same control you had before.
Severe gum disease can cause blood sugar spikes that last for hours after the initial infection or flare-up. Many diabetics notice their glucose readings become more erratic when they're dealing with dental problems, even if they're following their usual diet and medication schedule perfectly.
Breaking this cycle requires addressing both conditions simultaneously. Treating gum disease often leads to better blood sugar control, while improving glucose management helps your gums heal and stay healthy. Dental cleanings and periodontal treatments can actually help stabilize your diabetes management over time.
Regular dental visits become even more critical when you have diabetes because catching gum disease early prevents it from sabotaging your blood sugar control.
Common Oral Health Problems Diabetics
Experience
Increased Risk of Gum Disease and Periodontitis
Diabetes creates the perfect storm for gum problems. When blood sugar levels stay high, sugar gets into your saliva, feeding harmful bacteria in your mouth. These bacteria multiply rapidly, forming sticky plaque that irritates your gums and causes inflammation.
The relationship works both ways - diabetes makes gum disease worse, and gum disease makes blood sugar harder to control. People with diabetes face a 3-4 times higher risk of developing severe gum disease compared to those without diabetes. Early signs include red, swollen, or bleeding gums, but without proper care, this can progress to periodontitis.
Periodontitis is serious business. The infection spreads below the gum line, destroying the tissues and bones that support your teeth. Your gums may start pulling away from your teeth, creating pockets where more bacteria can hide. Eventually, this can lead to tooth loss.
Slower Healing After Dental Procedures
Your body's healing process takes a major hit when diabetes is in the picture. High blood sugar levels interfere with your immune system's ability to fight infection and repair tissue damage. After routine dental work like cleanings, fillings, or extractions, the recovery time stretches much longer than normal.
Blood circulation problems, common in diabetes, mean less oxygen and nutrients reach the healing tissues in your mouth. White blood cells, your body's infection fighters, don't work as effectively when surrounded by excess glucose. This creates a double problem - wounds heal slowly and are more likely to get infected.
Even simple procedures like tooth extractions can become complicated. The extraction site may not close properly, bleeding might continue longer than expected, and the risk of developing a painful dry socket increases significantly.
Higher Susceptibility to Oral Infections
Diabetes weakens your immune system's defenses, making your mouth a breeding ground for various infections. Oral thrush, caused by an overgrowth of Candida fungus, appears frequently in people with poorly controlled diabetes. You might notice white patches on your tongue, inner cheeks, or roof of your mouth that can be wiped away, leaving red, sore areas underneath.
Bacterial infections also take hold more easily. Abscesses - painful pockets of pus - can form around infected teeth or gums. These infections can spread quickly and become life-threatening if not treated promptly.
Viral infections like cold sores tend to be more severe and last longer in diabetics. The usual minor irritation becomes a more serious concern, often requiring prescription medications rather than healing on their own.
Dry Mouth and Its Cascading Effects
Many people with diabetes experience xerostomia, or dry mouth, due to decreased saliva production. This happens because high blood sugar levels cause frequent urination, leading to dehydration. Certain diabetes medications can also reduce saliva flow as a side effect.
Saliva plays a critical role in oral health - it washes away food particles, neutralizes acids produced by bacteria, and contains natural antibiotics. When saliva production drops, your mouth becomes vulnerable to a cascade of problems.
Without enough saliva, plaque builds up faster on your teeth and gums. Food particles stick around longer, feeding harmful bacteria. Your mouth's natural pH balance shifts toward acidic, creating an environment where tooth decay thrives. Many people with dry mouth also experience bad breath, difficulty swallowing, and changes in taste.
The lack of saliva's protective coating makes your tongue and cheeks more prone to injuries from normal activities like eating or speaking. These small wounds heal slowly and can become infected more easily in the diabetes-compromised environment.
Managing Blood Sugar for Better Oral Health
Maintaining stable glucose levels to protect your gums
Your blood sugar levels directly impact the health of your gums and teeth. When glucose levels spike consistently, your saliva becomes a breeding ground for harmful bacteria that love to feast on sugar. This creates a perfect storm for gum inflammation, bleeding, and eventual periodontal disease.
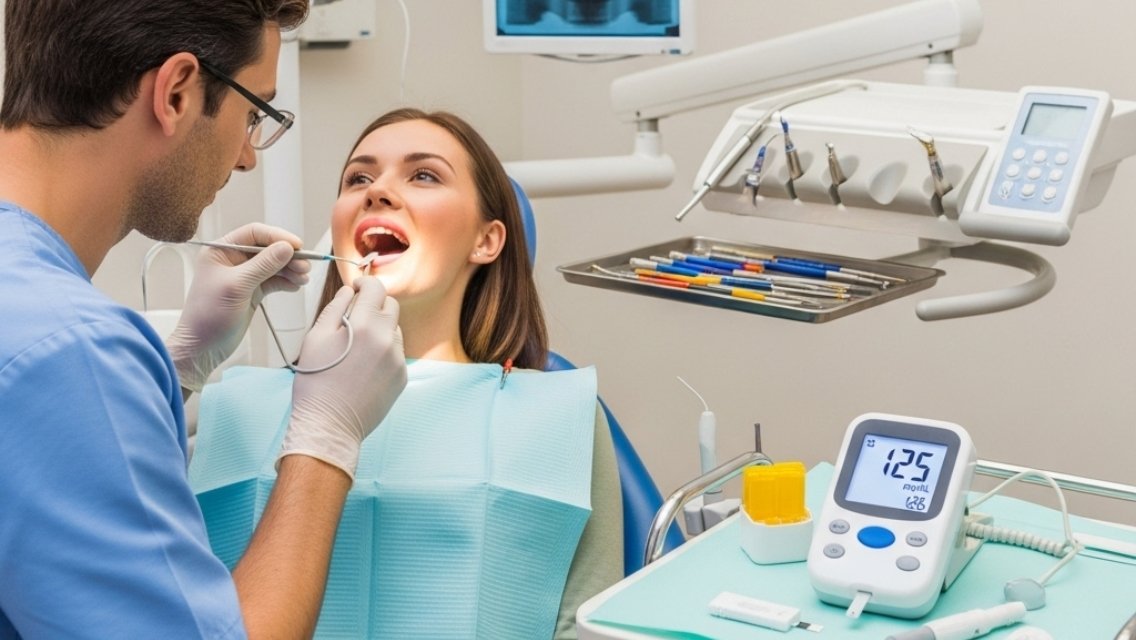
The sweet spot for blood sugar control sits between 80-130 mg/dL before meals and less than 180 mg/dL two hours after eating. Staying within these ranges helps reduce the amount of glucose in your saliva, making your mouth less hospitable to destructive bacteria. Your gums respond positively to stable glucose levels by maintaining their natural pink color, firm texture, and healthy barrier function against infection.
Regular blood sugar monitoring becomes your best defense against oral complications. Check your levels at least four times daily, especially before meals and bedtime. Keep a log of your readings alongside any oral symptoms you notice. This pattern tracking helps you identify which glucose levels trigger gum sensitivity, dry mouth, or increased plaque buildup.
Timing dental appointments with your blood sugar schedule
Smart scheduling of dental visits can make the difference between a comfortable appointment and a stressful experience. Your blood sugar patterns throughout the day should guide when you book cleanings, fillings, or more extensive procedures.
Morning appointments work best for most diabetics because blood sugar levels tend to be more stable after overnight fasting. Schedule routine cleanings between 9-11 AM when your medication has had time to work but before afternoon glucose fluctuations begin. Avoid late afternoon slots when blood sugar often dips, leaving you feeling shaky or weak during treatment.
Before any dental procedure, eat a normal meal 2-3 hours prior to maintain steady glucose levels. Bring your glucose meter and a quick-acting carbohydrate snack like glucose tablets or juice boxes. Tell your dentist if you're feeling symptoms of low blood sugar - sweating, shakiness, or confusion - so they can pause treatment.
For major procedures requiring sedation or extended time in the chair, coordinate with your endocrinologist about medication timing. Some procedures may require adjusting your insulin schedule or switching to shorter-acting medications temporarily.
How medication adjustments can improve oral outcomes
Your diabetes medications play a bigger role in oral health than you might realize. Different types of diabetes drugs affect your mouth in various ways, and working with your healthcare team to optimize your regimen can dramatically improve your dental outcomes.
Metformin, the most common Type 2 diabetes medication, sometimes causes a metallic taste or dry mouth. If you're experiencing these side effects, ask your doctor about splitting doses or trying extended release versions. Staying well-hydrated and using sugar-free gum can help stimulate saliva production.
Insulin users should pay special attention to timing and dosing around dental appointments. Long-acting insulin provides steady background coverage that protects your gums throughout the day. Short-acting insulin before meals prevents post-meal sugar spikes that feed oral bacteria. Work with your endocrinologist to fine-tune your insulin-to-carbohydrate ratios - better post-meal glucose control means healthier gums.
Some newer diabetes medications like GLP-1 agonists can cause nausea, affecting your eating schedule and potentially disrupting blood sugar patterns. If you're experiencing medication side effects that impact your ability to maintain good oral hygiene or regular eating schedules, discuss alternatives with your doctor.
Blood pressure medications often prescribed alongside diabetes drugs can cause dry mouth, increasing your risk of cavities and gum disease. Your healthcare team can adjust dosages or switch medications to minimize oral side effects while maintaining good diabetes and blood pressure control.
Essential Oral Care Strategies for Diabetics
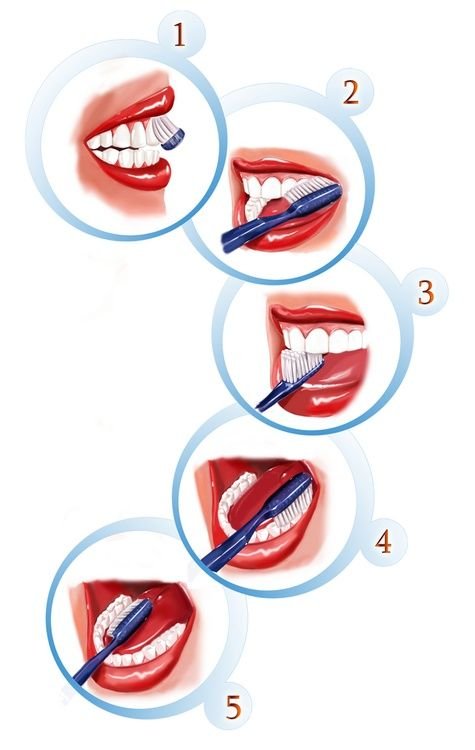
Modified brushing and flossing techniques for sensitive gums
Diabetics often deal with tender, inflamed gums that bleed easily during routine cleaning. The key is switching to gentler techniques that still maintain thorough plaque removal. Use a soft-bristled toothbrush and hold it at a 45-degree angle to your gum line. Instead of aggressive scrubbing, use small circular motions with light pressure. Electric toothbrushes with pressure sensors work particularly well since they prevent over-brushing while ensuring consistent cleaning.
For flossing, traditional string floss might feel too harsh on sensitive gums. Water flossers provide an excellent alternative, using pulsating water to remove debris without mechanical irritation. If you prefer traditional floss, try waxed varieties or specially designed floss for sensitive gums. Slide the floss gently between teeth using a back-and-forth motion rather than snapping it down forcefully.
Consider the timing of your oral care routine as well. Some diabetics find their gums are less sensitive in the evening after blood sugar levels have stabilized throughout the day.
Choosing the right toothpaste and mouthwash for diabetic needs
Not all oral care products are created equal for diabetics. Look for toothpastes containing fluoride to strengthen enamel, which becomes more vulnerable due to frequent blood sugar fluctuations. Antimicrobial ingredients like triclosan or stannous fluoride help combat the increased bacterial growth common in diabetic mouths.
Avoid toothpastes with sodium lauryl sulfate (SLS) if you experience dry mouth, a common diabetic side effect. SLS can worsen mouth dryness and irritate sensitive tissues.
For mouthwash, alcohol-free formulations are your best bet. Alcohol-containing mouthwashes dry out your mouth and can actually increase bacterial growth over time. Choose therapeutic mouthwashes with antimicrobial properties rather than cosmetic ones that simply freshen breath. Mouthwashes containing xylitol help stimulate saliva production while fighting harmful bacteria.
Some diabetics benefit from prescription-strength fluoride rinses, especially if they experience frequent cavities or enamel erosion.
Professional cleaning frequency recommendations
Standard dental cleaning schedules don't always meet diabetic needs. While most people visit the dentist twice yearly, diabetics typically benefit from cleanings every three to four months. This increased frequency helps manage the accelerated plaque and tartar buildup that high blood sugar levels can cause.
Your dental hygienist can remove hardened plaque that home care can't address, preventing it from harboring bacteria that worsen gum disease. These frequent visits also allow your dental team to catch problems early, before they become serious complications.
Schedule cleanings when your blood sugar is well-controlled. If you're experiencing a period of poor glucose management, inform your dentist. They might recommend postponing non-emergency procedures until your levels stabilize, as healing is slower during high blood sugar periods.
Consider deep cleanings (scaling and root planing) if you show signs of advanced gum disease. These procedures remove bacteria from below the gum line and smooth root surfaces to prevent future bacterial accumulation.
When to seek emergency dental care
Diabetics face unique situations that require immediate dental attention. Persistent mouth pain that doesn't respond to over-the-counter pain relievers could signal a serious infection that might spread rapidly in diabetic patients.
Watch for signs of dental abscesses: severe throbbing pain, facial swelling, fever, or a bitter taste in your mouth. These infections can become life-threatening for diabetics because high blood sugar impairs the immune system's ability to fight bacteria.
Seek immediate care for any oral injury that won't stop bleeding. Diabetics often have slower clotting times, making even minor cuts potentially problematic. Similarly, any loose or knocked-out teeth require urgent attention to prevent infection.
Sudden changes in your bite, severe dry mouth that develops quickly, or white patches in your mouth that don't brush away also warrant emergency visits. These could indicate serious complications like oral thrush or other infections that diabetics are particularly susceptible to developing.
Don't wait if you notice a bad taste or smell in your mouth accompanied by pain - these often signal brewing infections that need immediate antibiotic treatment.
Diabetes creates a two-way street when it comes to your mouth's health. High blood sugar levels make you more likely to deal with gum disease, dry mouth, and slower healing after dental procedures. At the same time, infections in your mouth can make it harder to control your blood sugar, creating a cycle that affects your overall well-being.
The good news is that you can break this cycle with the right approach. Keep your blood sugar levels steady, brush and floss regularly, and don't skip those dental checkups. Pay attention to warning signs like bleeding gums, persistent bad breath, or sores that won't heal. Talk to both your doctor and dentist about your diabetes so they can work together to keep your mouth and body healthy. Taking care of your oral health isn't just about having a nice smile – it's a key part of managing your diabetes successfully.